What is Degenerative Joint Disease?
Degenerative Joint Disease (DJD), often referred to as “osteoarthritis”, is a very common cause of lameness in performance horses. Most equine training strategies involve the prevention and/or maintenance of some form of joint disease. Lack of performance as a result of joint disease often precedes overt lameness and/or radiographic changes.
How many different types of joints are there?
There are 3 types of joints that are classified according to their range of motion. Synarthroses are immovable joints. Amphiarthroses move slightly. Diarthroses are movable joints. Most of the joints in the equine limb are diarthrodial in nature and are generally the ones we associate with equine lameness. Diarthrodial joints will therefore be described for the purpose of this discussion.
What structures make up a joint?
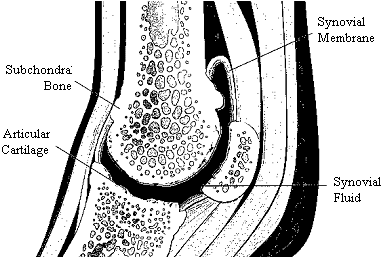
The synovial or diarthrodial joint consists of:
- articulating surfaces of bone (called subchondral bone)
- cartilage layer (overlying the subchondral bone)
- a fibrous joint capsule
- synovium (consisting of synovial membrane and fluid )
- associated supporting ligaments
The combination of a smooth cartilage surface and thick synovial fluid provides a low-friction environment through which the articulating surfaces can move freely and independently of each other.
What makes synovial fluid so thick and slippery?
Within synovial membrane and fluid is a large molecule called hyaluronan. Hyaluronan is the primary component of synovial fluid which gives it its thick and slippery characteristics. Since minimizing friction is critical to normal joint function, the presence of normal hyaluronan within a joint is very important. Lack of hyaluronan within synovial fluid increases friction associated with the synovial membrane and articular surfaces, therefore predisposing cartilage to excessive wear and erosion.
What causes joint inflammation (arthritis)?
Joint inflammation is a consequence of joint injury and/or instability. Instability can occur as a result of compromise of the supporting structures of the joint (such as the collateral ligaments), loss of articular cartilage (as may occur in osteochondrosis), overuse, and/or increased age.
The majority of the nerve endings lie within the fibrous capsule and supporting ligaments of the joint. There is very little sensitivity in the cartilage and synovium.
The three primary causes of joint pain, therefore, are:
- Joint effusion (i.e. increased fluid within the joint) resulting in distension/”stretching” of the joint capsule,
- Fibrosis/scarring of the joint capsule (often referred to as “capsulitis”), and
- Inflammation within the associated supporting ligaments of the joint (called “desmitis”)
Eliminating excess synovial fluid, inflammation within the fibrous capsule, and inflammation within the supporting ligaments will usually produce a comfortable joint.
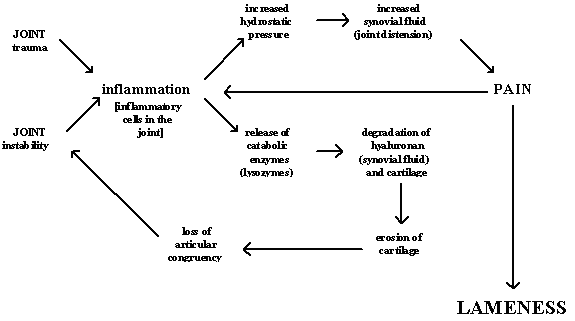
How does degenerative joint disease (DJD) occur?
The degenerative cycle is initiated as a result of joint instability and/or injury. Inflammation of the synovial membrane (a condition called synovitis) occurs secondary to joint instability/ trauma.
Inflammatory cells within the synovial membrane and fluid do two things:
- Their presence increases the hydrostatic pressure within the joint and
- They release catabolic enzymes (lysozymes) and other chemical mediators into the joint.
The increased hydrostatic pressure results in the influx of fluid into the joint (synovial effusion), distension (“stretching”) of the joint capsule, and pain. The enzymes released by the inflammatory cells degrade hyaluronan (the molecule that is involved in normal lubrication of the joint) as well as the cartilage layer. Compromise and eventual erosion of the cartilage layer results in loss of articular congruency, which in turn increases joint instability.
Interestingly, the presence of pain also accentuates the activity/release of harmful chemical mediators into the joint. Increased joint instability, the persistence of chemical mediators within the joint, and pain result in an increased inflammatory reaction.
And the cycle begins…
In order for a treatment strategy to be successful, it must focus on the following:How do we treat DJD?
- Maximizing joint stability
- Minimizing trauma to the joint
- Minimizing synovitis (joint inflammation)
- Minimizing synovial effusion (excessive joint fluid)
- Minimizing fibrosis of the joint capsule (which occurs as a result of chronic inflammation)
- Normalizing the joint environment (i.e. maximizing the amount of normal hyaluronan within the synovium)
- Minimizing pain
Currently, we have no effective way of stabilizing most diarthrodial joints without compromising their function and range of motion. Decreasing the challenge (i.e. the degree of extension/flexion) to the joints can often be achieved through corrective shoeing, however some degree of instability will usually persist. Surgery can be effective at improving joint stability and decreasing trauma in cases that involve developmental orthopedic lesions (such as osteochondrosis, OCD, subchondral cysts) and some types of fractures.
For the most part, however, we must rely on therapies designed to reduce inflammation and pain and normalize the synovial environment(s) as best as possible. These medications are referred to as “arthrotherapy”, and include both systemic and local forms.
What is SYSTEMIC arthrotherapy?
Any medication administered outside the joint (by mouth, intravenously, or intramuscularly for example) for the purpose of improving joint function and/or comfort is considered a form of systemic arthrotherapy. Anti-inflammatory medications (such as phenylbutazone), some pain relievers (such as capsaicin), and joint supplements (such as Adequan®, Legend®, and Cosequin®) are included in this category. Joint supplements have seen wide use in recent years, and are most often the client’s first line of treatment for DJD in their horse(s). The primary goal of the joint supplement is to stimulate normal activity and function of the synovial membrane thereby enhancing the integrity of the joint environment. Oral, intravenous, and intramuscular forms exist.
Most studies show that the oral medications (e.g. Cosequin®, MSM, Flex Free®, Corta-flex®, Synovi-G3, etc.) are quite effective when absorbed into the system. This type of arthrotherapy works especially well in people and dogs, which are able to absorb relatively large molecules (like glucosamine and chondroitin sulfate) through their intestinal wall easily. Horses, on the other hand, are generally not proficient at absorbing large molecules into their system from the intestinal tract. Therefore, a portion of the oral medication (and the client’s investment) may not be completely utilized. Many companies are continually working to find ways to improve absorbability of oral supplements in the horse.
Medications which bypass the intestinal tract of horses (and therefore do not rely on intestinal absorption) are generally preferred at present. These are injectable and include both prophylactic and therapeutic forms.
The South Shore Equine Clinic & Diagnostic Center recommends prophylactic arthrotherapy for the following:
- In horses with no current evidence of joint disease. The purpose of the medication is to delay the onset of DJD
- In horses with mild joint disease. The purpose of the medication is to alleviate symptoms enough for the horse to perform well in his/her intended capacity
- In horses with moderate to severe joint disease that have previously been treated with local therapy (i.e. injection). The purpose of the medication is to prolong the effect of the injection and delay the recurrence of clinical signs.
Prophylactic medications include Adequan®, Acetylglucosamine, Chondroprotec®, and Glucosamine (among others). Most treatment protocols involve one injection (5cc or 500mg) in the muscle once weekly for 4 consecutive weeks and then once or twice monthly thereafter (indefinitely). Cost varies anywhere from $25 to $65 per dose.
The South Shore Equine Clinic & Diagnostic Center recommends therapeutic arthrotherapy for the following:
- 36-48 hours prior to a race, clinic, or show. The purpose of the medication is to maximize the performance of the horse for a selected event.
Therapeutic medications such as Legend® are generally administered intravenously (in the vein). The cost of a single dose can range from $75 to $95. If regular (therapeutic) systemic treatment is required to produce and/or maintain soundness or does not result in a satisfactory response, then local arthrotherapy may be considered.
Local arthrotherapy typically involves injection of medication(s) directly into the joint. Typically, a combination of synthetic hyaluronan and steroid are infused. The steroid is extremely effective at eliminating inflammation (the presence of inflammatory cells) from within the joint. When the inflammatory cells leave, the hydrostatic pressure within the joint decreases, the excess fluid within the joint leaves, the joint capsule decompresses, and the discomfort is eliminated. Intraarticular steroids, therefore, are extremely effective at improving joint comfort.
On the other hand, steroids also promote the degradation of hyaluronan, the molecule that makes synovial fluid thick and slippery. Degradation of hyaluronan results in poor synovial fluid consistency, loss of protection of the cartilage layer, and accelerated joint degeneration. Therefore, steroids also have a deleterious effect to the joint environment.
Synthetic hyaluronan is typically infused concurrently into the joint to combat the degradative effects of steroid. Although synthetic hyaluronan doesn’t provide very much lubrication by itself, its presence in the joint stimulates the synovial membrane to produce more normal (endogenous) hyaluronan, thereby indirectly improving joint integrity.
It is very important to determine which is the lesser of two evils: 1) allowing the presence of inflammatory cells and their degradative effects to persist within the joint or 2) face the consequences of infusing steroid into the joint. In some cases, infusing steroid into the joint is the healthiest choice. Making the right decision becomes particularly critical in regard to high-motion (diarthrodial) joints, where a little joint degeneration can go a long way.